When you hear CTE, your mind probably jumps to professional football players. That’s where the public conversation started, but it’s also where many myths took root. The truth about this complex brain condition is much broader, affecting more people than you might realize. Understanding the real CTE symptoms requires looking past the headlines and focusing on the facts. This guide will clear up the common misconceptions about who is at risk and how the condition is diagnosed, giving you the solid foundation you need to make informed decisions for your family.
Key Takeaways
- CTE develops from cumulative head trauma, not a single injury: This brain disease is caused by the long-term effects of repeated head impacts, with symptoms like memory loss and mood changes often appearing years or decades later.
- Symptom management is the key to treatment: Since there’s no cure, the focus is on improving quality of life through a personalized plan of medication, therapy, and a strong support system for both the individual and their caregivers.
- Negligence has legal consequences: While preventing head injuries is the best approach, you may have legal options if an organization’s failure to protect you or a loved one contributed to the condition. It’s essential to act quickly due to strict deadlines for filing claims.
What is Chronic Traumatic Encephalopathy (CTE)?
Chronic Traumatic Encephalopathy, or CTE, is a serious brain disease that develops after repeated head injuries. It’s a neurodegenerative condition, which is a clinical way of saying that brain cells slowly become damaged and die over time. Unlike a single severe concussion, CTE is the result of a cumulative history of head trauma. This includes both concussive and sub-concussive hits—impacts that don’t cause obvious symptoms but still jolt the brain. Because it’s a progressive disease, the damage gets worse as the years go by, long after the initial injuries have stopped.
This condition is often associated with athletes in contact sports like football and boxing, as well as military veterans exposed to blast injuries. However, it can affect anyone who has experienced repetitive head trauma. What makes CTE particularly challenging is that its symptoms often don’t show up for years or even decades. This long delay can make it incredibly difficult to connect the later health problems back to the head injuries that caused them. Understanding this condition is the first step toward recognizing its impact and knowing what to look for if you or a loved one has a history of head trauma.
What Does CTE Do to the Brain?
CTE fundamentally changes how a person thinks, feels, and moves by destroying nerve cells in the brain. The symptoms typically begin subtly, often 8 to 10 years after the head injuries stop. Early signs might include confusion, dizziness, and headaches. As the disease progresses, the effects become more severe. You might notice significant memory loss, impulsive behavior, and poor judgment. Eventually, CTE can impact physical abilities, leading to problems with balance, speech, and coordinated movement. These changes can be confusing and distressing for both the individual and their family, as they slowly alter a person’s personality and ability to function independently.
What Is Tau Protein’s Role in CTE?
The damage in CTE is linked to a protein in our brain called tau. Normally, tau helps stabilize the internal structure of our brain’s nerve cells. However, researchers believe that repeated head trauma can trigger a chain reaction, causing tau proteins to misfold and clump together. These abnormal tau clumps spread throughout the brain, disrupting communication between cells and eventually killing them. This process also causes the brain to shrink. While other conditions like Alzheimer’s disease also involve tau, the pattern of its buildup in CTE is unique. This buildup is what drives the progressive decline in brain function seen in individuals with the disease.
The Unique Pattern of Tau Protein Buildup
What really sets CTE apart from other brain diseases like Alzheimer’s is how and where the tau protein accumulates. In a brain with CTE, the abnormal tau doesn’t just spread out randomly. Instead, it forms a distinctive pattern, collecting in clumps around the small blood vessels deep within the brain’s folds. This specific location is a tell-tale sign for neuropathologists. This buildup of tau protein disrupts the normal function of brain cells, leading to their death and causing the brain to shrink over time. It’s this unique signature that allows for a definitive diagnosis of CTE after death and helps researchers understand how repetitive head trauma specifically damages the brain.
What Causes CTE and Who Is at Risk?
Understanding what causes Chronic Traumatic Encephalopathy (CTE) is the first step toward recognizing its impact. Unlike a traumatic brain injury from a single event, CTE develops from a history of repeated head trauma. The condition is a progressive neurodegenerative disease, meaning it gradually damages and destroys brain cells over time. While anyone can sustain a head injury, certain groups face a significantly higher risk due to the nature of their work or activities. Identifying these risk factors is key to prevention and early awareness. If you or a loved one falls into one of these categories, knowing the signs can make all the difference.
Connecting Repetitive Head Trauma to CTE
The primary cause of CTE is repeated head trauma. This includes both concussions that cause noticeable symptoms and, just as importantly, sub-concussive hits—smaller impacts that may not seem serious at the time. Over years, the cumulative effect of these hits can trigger changes in the brain. Specifically, they lead to the buildup of an abnormal protein called tau, which forms clumps that slowly spread and kill brain cells. This process disrupts normal brain function, leading to the cognitive, behavioral, and mood-related symptoms associated with Chronic Traumatic Encephalopathy. It’s the repetitive nature of the injuries, rather than their individual severity, that is the defining factor in developing CTE.
Which Sports Pose the Highest Risk?
Athletes who participate in certain contact sports are among the most well-known groups at risk for CTE. The risk is highest in sports where hits to the head are a routine part of play, practice, and competition. This includes athletes in football, ice hockey, boxing, rugby, mixed martial arts, and even professional wrestling. The constant jarring and impacts, season after season, create the exact conditions that can lead to CTE later in life. It’s important for athletes, coaches, and families to be aware of these risks and prioritize safety protocols to minimize head impacts whenever possible.
The Risk for Veterans: Military Service and Blast Exposure
Our military service members also face a significant risk of developing CTE, particularly those who have been in combat. The danger often comes from exposure to explosive blasts from IEDs or other devices. The shockwave from a blast can cause the brain to move violently within the skull, leading to injury even without a direct blow to the head. Like in sports, repeated exposure to these events increases the risk. Veterans who have experienced blast exposure or other head trauma during their service should be aware of the potential long-term effects and monitor for any emerging symptoms of CTE.
Genetic and Statistical Risk Factors
While a history of head impacts is the main ingredient for CTE, it doesn’t tell the whole story. Two people can have similar athletic or military careers, yet only one might develop the disease. This has led researchers to investigate other contributing factors, including genetics. Some studies suggest that certain genetic variations may make a person more susceptible to the brain changes seen in CTE after head trauma. Beyond genetics, other statistics matter, too. The number of years spent in a high-contact sport and the age at which a person first started playing can also significantly influence their long-term risk. Understanding these factors helps create a clearer picture of who is most vulnerable and why proactive monitoring is so important.
What Are the Symptoms of CTE?
Recognizing the symptoms of Chronic Traumatic Encephalopathy (CTE) can be difficult because they often don’t appear until years, or even decades, after the head injuries occurred. The signs are usually subtle at first and can easily be mistaken for other conditions, like normal aging or different neurological disorders. Symptoms generally fall into four main categories: cognitive, behavioral, mood, and motor. Understanding these is the first step toward getting help and exploring your options.
The progression of CTE varies from person to person, but it is a degenerative disease, meaning it typically worsens over time. What might begin as minor memory lapses or irritability can develop into more severe issues that impact every aspect of a person’s life, from their ability to work to their personal relationships. These symptoms can have a profound and devastating impact, sometimes leading to complex personal injury cases when the injuries are linked to negligence. If you or a loved one has a history of head trauma and are experiencing these changes, understanding the potential connection is crucial for both health and legal reasons.
Two Patterns of Symptom Onset
The way CTE symptoms appear generally follows two distinct patterns. First, there is often a long delay between the head injuries and the first signs of the disease. Symptoms typically begin subtly, sometimes 8 to 10 years after the repetitive trauma has ended, making it difficult to connect the issues back to a past sports career or military service. The second pattern is the progressive nature of the condition. Because CTE is a degenerative disease, once symptoms appear, they tend to worsen over time. What might start as minor irritability or forgetfulness can develop into severe cognitive and behavioral problems, fundamentally changing a person’s ability to function and interact with the world.
Spotting the Early Warning Signs
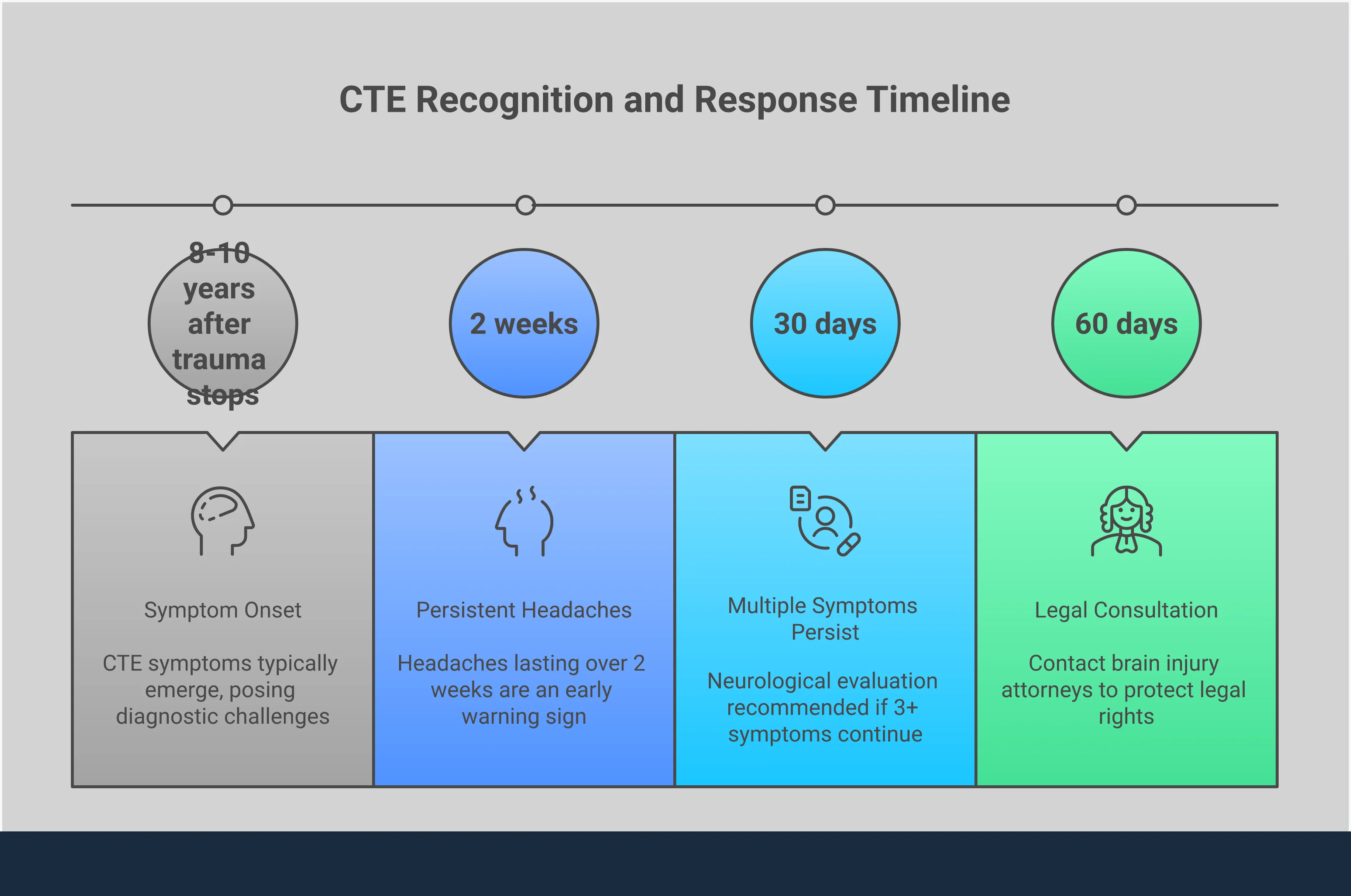
The earliest signs of CTE are often easy to dismiss. Symptoms typically begin to surface 8 to 10 years after the repetitive head trauma occurred. Initially, a person might experience persistent headaches, dizziness, and a general sense of confusion or feeling “in a fog.” Because these symptoms are so common and can be attributed to many other causes, they are frequently overlooked. However, when there’s a history of concussions or repeated blows to the head—whether from sports, military service, or an accident—these early indicators shouldn’t be ignored. They represent the first subtle changes happening in the brain as the condition begins to take hold, and paying attention to them is key.
How CTE Affects Cognition and Memory
As CTE progresses, cognitive difficulties become more pronounced. One of the most common symptoms is memory loss, particularly with short-term memory. A person might forget conversations they just had, misplace important items, or struggle to recall recent events. Beyond memory, CTE affects executive functions—the mental skills that help you plan, organize, and get things done. This can show up as trouble solving problems, making sound decisions, or creating a simple plan. These cognitive declines can make it challenging to manage daily responsibilities, maintain employment, and handle personal finances, creating significant stress for the individual and their family.
Recognizing Changes in Behavior and Mood
Significant shifts in mood and behavior are hallmark symptoms of CTE, and they can be incredibly distressing for both the individual and their family. It’s common for someone with CTE to experience depression, anxiety, and apathy. Some may even have suicidal thoughts. Behaviorally, symptoms can include aggression, irritability, and poor impulse control, leading to uncharacteristic outbursts or erratic actions. These personality changes can strain relationships and lead to social isolation. Loved ones may feel like they are dealing with a completely different person, not realizing that a progressive brain injury is the underlying cause of these deeply concerning changes.
Physical and Motor Symptoms to Watch For
In the later stages of CTE, physical symptoms begin to emerge as the damage to the brain becomes more widespread. These are often similar to symptoms seen in other neurodegenerative diseases like Parkinson’s. Motor problems can include tremors, slowed movement, and muscle stiffness. A person’s walk may become unsteady, which increases their risk of falling and further injury. Speech can also be affected, becoming slurred or difficult to understand (dysarthria). As the condition advances, these physical impairments can lead to a significant loss of independence, often requiring more intensive, round-the-clock care and support from family members or professionals.
How Is CTE Diagnosed?
Getting a clear diagnosis for Chronic Traumatic Encephalopathy (CTE) is one of the biggest challenges families face. Unlike many other conditions, there isn’t a simple test or scan that can confirm CTE in a living person. The symptoms often mimic other neurological disorders, which can lead to years of uncertainty and misdiagnosis. This diagnostic gray area is frustrating for those experiencing symptoms and their loved ones who are trying to understand what’s happening.
Currently, the only way to get a definitive CTE diagnosis is through a post-mortem examination of brain tissue. However, medical professionals can make a clinical diagnosis in living individuals by carefully evaluating their symptoms and history. This involves piecing together a puzzle of cognitive changes, mood swings, and, most importantly, a documented history of repeated head impacts. While it’s not a final confirmation, a clinical assessment is the first step toward getting the right support and care. If you or a loved one has suffered head trauma due to an accident, understanding the diagnostic process is crucial for both your health and any potential personal injury claims.
Why Is CTE So Difficult to Diagnose?
One of the main reasons CTE is so difficult to diagnose is that its symptoms overlap significantly with other brain conditions, such as Alzheimer’s disease, Parkinson’s, and depression. A person experiencing memory loss, confusion, and mood changes could be dealing with any number of issues, making it tough for doctors to pinpoint CTE as the cause. Furthermore, standard brain imaging tests like MRIs and CT scans cannot detect the specific changes caused by CTE. These scans can rule out other problems like tumors or strokes, but they won’t show the telltale tau protein buildup that defines the disease. This lack of a clear biomarker in living patients is a major hurdle for the medical community.
Diagnosing Traumatic Encephalopathy Syndrome (TES)
Since a definitive CTE diagnosis can only be made after death, researchers and doctors developed criteria for what’s called Traumatic Encephalopathy Syndrome, or TES. This is the clinical diagnosis for the symptoms of CTE in a living person. Think of it as a framework doctors use to identify the condition based on the available evidence. The process involves a thorough evaluation, including a detailed review of the person’s history of head injuries and an assessment of their cognitive and behavioral symptoms. Doctors will also work to rule out other conditions that could be causing the symptoms. A TES diagnosis is made when there is a clear link between a history of head trauma and the specific pattern of problems the person is experiencing, giving families a name for what they’re facing and a path forward for care.
Confirming a Diagnosis Post-Mortem
The only way to be 100% certain that someone had CTE is by examining their brain after they have passed away. During an autopsy, a neuropathologist can slice and stain sections of brain tissue to look for clumps of an abnormal protein called tau. In CTE, these tau tangles have a unique pattern, typically gathering around the brain’s blood vessels in the depths of the cortex. This post-mortem analysis provides families with definitive answers and contributes valuable data to ongoing CTE research. While it doesn’t help the individual who suffered, it can bring closure and a better understanding of the symptoms they experienced in life.
How Does CTE Differ from Other Brain Conditions?
While a definitive diagnosis isn’t possible while someone is alive, doctors can still form a strong clinical suspicion of CTE. They do this by conducting a comprehensive evaluation. This includes a detailed review of the person’s medical history, with a special focus on any past head injuries from sports, military service, or accidents. They will also perform physical and neurological exams to assess memory, concentration, and motor skills. By carefully ruling out other conditions and connecting the symptoms to a history of head trauma, a doctor can conclude that CTE is the most likely cause, allowing the patient and their family to move forward with a plan for managing symptoms.
Co-Occurring Brain Diseases
It’s important to understand that CTE doesn’t always exist in isolation. The damage from repeated head trauma can create a complicated medical picture, and it’s not uncommon for someone with CTE to also show signs of other neurodegenerative conditions. People with CTE might also develop diseases like Alzheimer’s, ALS, or Parkinson’s. While some of these conditions also involve the tau protein, the way it builds up in CTE is distinct—it clusters around blood vessels in a unique pattern. This overlap of symptoms can make a diagnosis even more challenging for families. In fact, research shows that brain injuries sustained earlier in life can make a person two to four times more likely to develop dementia later on, highlighting how one form of brain trauma can open the door to multiple issues down the road.
How Does CTE Progress Over Time?
CTE is a progressive disease, meaning its effects worsen over time. Unlike an injury with immediate and obvious consequences, the damage from CTE unfolds slowly, often over the course of many years. Understanding this progression is key for families trying to make sense of the changes they’re seeing in a loved one. The disease is typically broken down into distinct stages, each with its own set of challenges.
What Is the Typical Timeline for CTE Symptoms?
One of the most challenging aspects of CTE is the long delay between the head injuries and when symptoms first appear. According to research, the initial symptoms of CTE usually don’t show up until 8 to 10 years after a person has experienced repeated head trauma. This gap can make it incredibly difficult to connect the dots between a past football career or military service and the current struggles with memory or mood. Because the onset is so gradual, early signs are often dismissed as normal aging or stress, delaying a potential diagnosis and the search for supportive care.
Breaking Down the Four Stages of CTE
As CTE advances, it moves through four general stages. In the beginning, the changes can be subtle.
- Stage 1: A person might experience mild headaches, confusion, and feel a bit disoriented.
- Stage 2: The symptoms become more pronounced. This stage often brings memory loss, poor judgment, and impulsive behavior that can strain relationships.
- Stages 3 & 4: In the later, more severe stages, the condition can lead to dementia. According to the Cleveland Clinic, individuals may develop serious movement problems like tremors, have trouble speaking, and face deep depression or anxiety. These advanced stages require significant care and support for both the individual and their family.
Understanding the Long-Term Outlook
The long-term outlook for someone with CTE is challenging because it is a progressive condition where symptoms inevitably worsen over time. While the speed of this decline varies from person to person, CTE is a degenerative disease that gradually erodes an individual’s abilities and independence. What might begin as minor memory lapses or uncharacteristic irritability can develop into severe cognitive and behavioral problems that impact every aspect of a person’s life, from their career to their family relationships. In the most advanced stages, the condition often leads to dementia, requiring round-the-clock care. This slow, heartbreaking progression places an immense emotional and financial burden on families, highlighting the importance of planning for future care and understanding all available support options.
How Can You Treat CTE?
Receiving a CTE diagnosis, or suspecting you or a loved one has it, can feel overwhelming. While there is currently no cure for CTE, there are effective ways to manage the condition. The brain damage cannot be reversed, but a proactive approach to CTE treatment can significantly improve a person’s quality of life. Because CTE affects everyone differently, treatment plans are highly personalized, often combining medication, therapy, and strong supportive care. This strategy is similar to how other neurodegenerative conditions are managed, focusing on symptom relief and stability.
Can Medication Help Manage Symptoms?
Medication is a key part of a CTE treatment plan, but it’s used to manage symptoms, not to cure the disease. For example, if someone is struggling with mood changes like depression or anxiety, a doctor might prescribe antidepressants. For those experiencing memory loss or cognitive difficulties, certain drugs used for Alzheimer’s disease may be recommended to help with focus. Medications can also help manage irritability and sleep disturbances. It’s essential to work closely with a medical professional to find the right medication and dosage for your specific needs.
Specific Medications for Symptom Management
To address the wide range of symptoms, doctors may prescribe several types of medication. For the emotional and mood-related challenges, such as depression or anxiety, Selective Serotonin Reuptake Inhibitors (SSRIs) are a common choice. When it comes to cognitive issues like memory loss, cholinesterase inhibitors—often used in Alzheimer’s treatment—can sometimes help with focus. For more difficult behavioral and cognitive problems, including severe irritability or aggression, a doctor might consider atypical antipsychotics. The goal is always to create a personalized medication plan that targets specific symptoms, making daily life more manageable. This approach requires close partnership with a healthcare provider to find the right balance and improve overall quality of life.
The Role of Therapy and Rehabilitation
Therapy is a cornerstone of managing CTE and can make a huge difference in daily life. Different types of therapy target specific challenges. For instance, cognitive behavioral therapy (CBT) helps individuals develop coping strategies for mood swings and anxiety. Occupational therapy focuses on adapting daily routines to make tasks easier and safer. If motor skills are affected, physical therapy can improve balance, and speech therapy can help with communication. These therapies empower individuals by giving them practical tools to handle their symptoms.
Why Supportive Care Is Essential
Beyond medical treatments, a strong support system is vital for anyone living with CTE. This involves creating a safe and stable environment at home. Family members and caregivers play a crucial role in providing emotional support and practical assistance. Simple strategies, like maintaining a consistent daily routine, reducing clutter to prevent falls, and using calendars as memory aids, can be incredibly helpful. Support groups, for both the individual and their caregivers, also provide a sense of community and a space to share experiences.
The Importance of Legal and Financial Planning
As CTE progresses, the cognitive and behavioral changes can make it difficult for a person to manage their finances or make critical healthcare decisions. Planning ahead is one of the most important steps you can take. Setting up legal documents, such as a power of attorney and a healthcare directive, ensures that your loved one’s wishes are respected and their affairs are handled properly. Beyond future planning, it’s also important to consider how the injuries occurred. If the head trauma was a result of another party’s negligence, you may be entitled to compensation to help cover medical bills and long-term care. Because there are strict deadlines for filing personal injury claims, it’s wise to understand your legal options as soon as possible.
Can You Prevent CTE?
While there’s no guaranteed way to prevent Chronic Traumatic Encephalopathy, you can take meaningful steps to lower the risk. The most effective strategy is straightforward: reduce the frequency and severity of head impacts. This involves improving safety rules in high-contact activities, using protective equipment correctly, and knowing how to respond when a head injury occurs. By focusing on these key areas, athletes, parents, and coaches can create a safer environment and make informed decisions about long-term health.
Making Sports Safer to Reduce Risk
The most important step in preventing CTE is to limit an athlete’s exposure to head trauma. Many sports organizations are now implementing rule changes and new safety measures to do just that. For example, leagues have introduced stricter penalties for illegal hits, revised tackling rules in football to discourage leading with the helmet, and limited contact in practices. These changes aim to protect players by altering how the game is played, shifting the focus toward skill over brute force. The goal is to preserve the sport while prioritizing the long-term health of its participants.
Protective Gear and Protocols That Matter
Protective gear like helmets and mouthguards plays a vital role in preventing injuries like skull fractures. However, it’s crucial to understand their limitations. There isn’t strong evidence that current helmet technology prevents concussions or the hits that lead to CTE, though they do help reduce impact forces. This is why safety protocols are just as important as the equipment. Enforcing proper tackling techniques, teaching players to keep their heads up, and ensuring equipment fits correctly are all essential parts of a comprehensive safety plan.
What to Do After a Head Injury
Knowing how to react after a head injury is critical. Any athlete suspected of having a concussion should be removed from play immediately. The old “shake it off” mentality is dangerous and has no place in sports today. An athlete must be given time to fully recover before returning, as a second impact during this period can be devastating. If coaches or organizations fail to follow concussion protocols and an athlete suffers further harm, there can be serious consequences. Understanding your rights is key to ensuring accountability. If you believe safety protocols were ignored, exploring your legal options can help.
What Are Your Legal Options with CTE?
A CTE diagnosis brings a wave of emotional and financial challenges. While you focus on care and support for your loved one, it’s also important to understand your legal options. If the repeated head trauma that led to CTE was caused by another party’s negligence—like a sports league, school, or employer—you may be entitled to compensation. These cases are complex, often involving detailed medical evidence and a deep understanding of liability. However, they are essential for holding responsible parties accountable and securing the resources your family needs for future medical bills, long-term care, and lost income.
The legal process can feel overwhelming, especially when you’re already dealing with so much. But you don’t have to face it alone. An experienced attorney can help you understand the specifics of your situation, gather the necessary evidence, and guide you through every step of seeking justice. The first step is simply learning about the potential avenues available to you, from personal injury claims to workers’ compensation. Knowing your rights is the foundation for making informed decisions for your family’s future. It empowers you to take action and fight for the support you deserve.
Should You File a Personal Injury Claim?
If a loved one developed CTE due to someone else’s negligence, you may have legal options. A personal injury claim seeks to prove that an organization or individual failed in their duty to provide a safe environment, leading to the brain injuries that caused CTE. This could apply to sports organizations that didn’t enforce safety protocols or employers in high-risk fields who failed to protect their workers. A successful claim can help cover medical expenses, lost wages, and the immense pain and suffering your family has endured. Exploring your options with a firm that understands various practice areas is a crucial step toward getting the support you deserve.
Is Workers’ Compensation an Option?
For individuals who sustained head injuries on the job, such as professional athletes or military personnel, a workers’ compensation claim may be an option. Unlike a personal injury lawsuit, workers’ compensation is typically a no-fault system, meaning you don’t have to prove negligence. It is designed to provide medical benefits and wage replacement for injured employees. While these claims can provide necessary financial support, they also serve a larger purpose. CTE lawsuits have broader implications beyond individual compensation. They serve as catalysts for change, driving improvements in safety standards across entire industries and protecting others from similar harm in the future.
Don’t Miss the Deadlines for Legal Action
When it comes to legal action for CTE, time is a critical factor. Every state has a statute of limitations, which sets a strict deadline for filing a lawsuit. For CTE, this can be complicated because symptoms often don’t appear until years or even decades after the head injuries occurred. Determining when the clock starts ticking requires a careful legal analysis of your specific circumstances. Because of this complexity, it is vital to speak with an attorney as soon as you suspect CTE may be a factor. Don’t wait to contact a legal professional who can help you understand the deadlines and protect your right to seek justice.
Debunking Common Myths About CTE
When it comes to brain injuries, there’s a lot of information out there, and not all of it is accurate. Chronic Traumatic Encephalopathy (CTE) is often discussed in the news, usually in the context of professional sports, but this has created some common misunderstandings about the condition. Getting the facts straight is the first step toward understanding what you or a loved one might be facing. These myths aren’t just harmless trivia; they can prevent people from seeking the right medical care or exploring their legal options after an injury.
For families dealing with the confusing and often heartbreaking symptoms, these misconceptions can add another layer of difficulty. You might wonder if the changes you’re seeing are related to a past injury, but dismiss the idea because it doesn’t fit the popular narrative. Believing that only certain people are at risk or that symptoms should have appeared sooner can cause critical delays in getting support. It’s important to separate fact from fiction, especially when the consequences are so serious. Let’s clear up a few of the most persistent myths about CTE so you have the information you need. If you believe a head injury was caused by someone else’s negligence, knowing the truth about this condition is crucial for protecting your rights.
Myth: CTE Only Affects Professional Athletes
This is one of the biggest misconceptions about CTE. While the condition gained public attention through studies on former football players, it’s not limited to the pros. The reality is that CTE can affect anyone who has experienced repeated head trauma. This includes amateur athletes in sports like soccer, hockey, and boxing, as well as military veterans who have been exposed to blast injuries. It also includes individuals who have suffered from domestic violence, repeated falls, or other situations involving multiple head injuries. The key risk factor isn’t a professional contract; it’s the history of repeated impacts to the head over time.
Myth: Symptoms Show Up Immediately
Unlike a concussion, where symptoms can be immediate, the effects of CTE are often delayed. In fact, the symptoms of CTE typically don’t begin to show up until years, or even decades, after the head injuries occurred—often 8 to 10 years later. This long latency period can make it difficult to connect the symptoms back to the original trauma. An individual might start experiencing memory loss, mood swings, or confusion in their 40s or 50s, long after they stopped playing a sport or left military service. This delay is a defining and challenging feature of the disease.
Myth: CTE Can Be Diagnosed in Living Patients
Currently, there is no single test that can definitively diagnose CTE in a living person. The only way to confirm a CTE diagnosis is by examining brain tissue during an autopsy after death. While doctors can suspect CTE based on a person’s history of head trauma and their symptoms, a definitive diagnosis while they are alive isn’t possible. This is because the symptoms of CTE—like memory problems, depression, and impaired judgment—overlap significantly with other neurodegenerative conditions, such as Alzheimer’s disease. Researchers are actively working on developing diagnostic tools for the living, but for now, it remains a post-mortem diagnosis.
How to Find Support for Your Family
Caring for a loved one with CTE can feel isolating, but you don’t have to manage it on your own. The emotional, physical, and financial toll affects the entire family, making a strong support system essential. Finding the right resources can provide comfort, practical advice, and a sense of community with others who understand what you’re going through. From connecting with advocacy groups to seeking professional counseling, there are many ways to get the help you and your family need. Building this network allows you to share the burden, learn coping strategies, and find the strength to face the challenges ahead together.
Connecting with Support Groups and Advocates
Connecting with others who have firsthand experience with brain injuries can be incredibly validating. Support groups, whether online or in your local community, offer a safe space to share stories, exchange advice, and simply feel understood. If you’ve been affected by CTE, remember that you’re not alone. Advocacy organizations also play a crucial role by raising awareness and pushing for better safety measures in sports and other high-risk activities. In some cases, taking legal action is another form of advocacy. CTE lawsuits not only provide compensation for families but also serve as powerful catalysts for change, encouraging institutions to prioritize brain health and safety.
Prioritizing Mental Health with Counseling
The impact of a brain injury on a family can be profound, and it’s important to care for your own mental well-being. Professional counseling can provide you and your loved ones with effective coping strategies to handle the stress, grief, and uncertainty that often accompany a CTE diagnosis. A therapist specializing in chronic illness or brain injuries can help family members process complex emotions and prevent caregiver burnout. Family counseling can also improve communication and help everyone adapt to new roles and dynamics. Seeking support from a mental health professional is a proactive step toward building resilience for the journey ahead. The Brain Injury Association of America is an excellent resource for finding local support and services.
Related Articles
- Can Emotional Trauma Cause Brain Damage? The Proof
- How to Choose a Severe Injury Attorney in Kansas City – The Law Office of Chad G. Mann, LLC
- Personal Injury Lawyer Kansas City: Guide & Top Tips
- How to Pick a Workmans Comp Lawyer Springfield MO
Frequently Asked Questions
How is CTE different from a single bad concussion? Think of a concussion as a one-time event—a distinct injury with a recovery period. CTE, on the other hand, is the result of a long history of head impacts. It’s the cumulative damage from hundreds or thousands of hits over many years, including smaller, sub-concussive ones that didn’t cause any obvious symptoms at the time. The problem isn’t one single injury, but the repetitive trauma that triggers a slow, progressive decline in brain health.
My loved one played sports years ago and is now having memory problems. Could it be CTE? It’s a valid question, and it’s one that many families face. A key feature of CTE is the long delay between the head injuries and the first appearance of symptoms, which can be a decade or more. If your loved one has a history of contact sports or military service and is now showing changes in memory, mood, or behavior, it’s wise to consider CTE as a possibility. The first step is to schedule a thorough evaluation with a doctor to discuss their symptoms and full medical history.
What’s the first thing I should do if I think a family member has CTE? The most important first step is to seek a medical evaluation, preferably with a neurologist who has experience with brain injuries. Before the appointment, try to document the symptoms you’ve noticed and gather as much information as you can about your loved one’s history of head trauma. This process is about getting clarity and creating a plan to manage their symptoms and improve their quality of life. It also provides the medical documentation that is essential if you later decide to explore your legal options.
Is it possible to file a lawsuit for CTE if the injuries happened a long time ago? This is a common concern, as the time limits for filing lawsuits, known as statutes of limitations, can be complex. However, in many cases, the clock doesn’t start until the injury or condition is discovered. Because CTE symptoms often appear decades after the initial trauma, you may still have legal options. It’s crucial to speak with an attorney who can analyze the specifics of your situation and explain the deadlines that apply.
Can my child still play sports safely? Many parents worry about this, and it’s about finding a balance. While no contact sport is completely without risk, you can take steps to make it safer. This includes ensuring your child’s coaches teach proper techniques, enforce safety rules, and follow strict concussion protocols. The most critical rule is that any player suspected of having a concussion must be removed from play immediately and not return until cleared by a medical professional. Open communication with your child and their coaches is key to prioritizing their long-term health.
Immediate Help for Suicidal Thoughts
If you or someone you love is having thoughts of self-harm, this is a medical emergency that requires immediate action. The behavioral and mood changes associated with CTE can be overwhelming, but help is available right now. Do not wait. Call or text 988 in the United States to connect with the 988 Suicide & Crisis Lifeline for free, confidential support 24/7. You can also call 911 or go to the nearest emergency room. These resources are staffed by trained professionals who can provide immediate help and guidance in a crisis. Reaching out is the most important step you can take to ensure safety and get the support needed to handle these incredibly difficult moments.